Cell therapy trial holds promise for critical lung failure
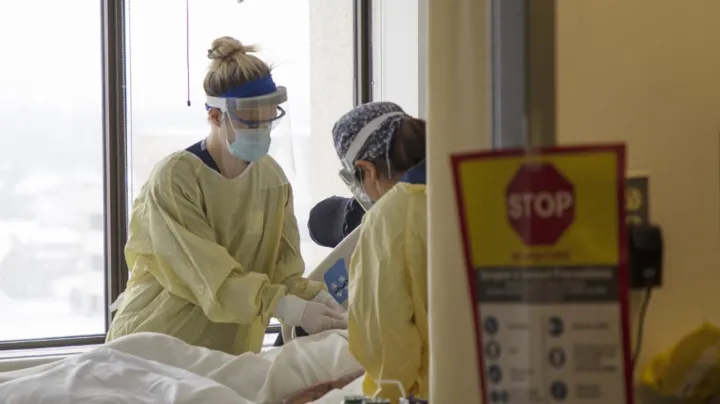
Researchers at The Ottawa Hospital translated discovery into treatment rapidly during the COVID-19 pandemic thanks to expertise in lab research, biomanufacturing and clinical trial design.
Every year, millions of people have life-threatening lung failure called acute respiratory distress syndrome (ARDS). This severe immune reaction to infection or trauma fills the lung’s air sacs with fluid. Treatments are limited, and it is often fatal.
When the pandemic hit and COVID-19-associated ARDS threatened to overwhelm ICUs, there was a push to find better treatments.
In March 2020, Drs. Duncan Stewart, Shane English, Dean Fergusson and colleagues at The Ottawa Hospital began planning an innovative clinical trial to see whether mesenchymal stem cells (MSCs), which can promote healing, could help treat severe COVID-19-associated ARDS. It built on a previous trial at The Ottawa Hospital that used MSCs to treat patients in severe septic shock.
The trial opened in record time that June, thanks to efficient teamwork by the hospital and research institute’s clinician and basic scientists, methodologists, research staff and biomanufacturing experts, as well as Health Canada’s rapid review of pandemic-related trials.
The results of this research, which included Phase 1 and 2 trials, were recently published in Stem Cell Reports.

“Despite the small number of patients recruited to the trial, we couldn’t have hoped for better results. We found MSCs have an important biological effect on these critically ill patients," said Dr. Duncan Stewart.
The Phase 1 trial of 15 patients showed the MSC treatment was safe with no side effects. The Phase 2 randomized controlled trial enrolled 22 patients, but was stopped early due to fewer cases of COVID-19-associated ARDS after vaccines were introduced.
The data the research team collected is promising. Patients who received MSCs showed consistent signs of improvement, such as fewer days on high levels of oxygen and better survival. They also had a full recovery of severely depressed white blood cell counts, which is a predictor of poor outcomes in ARDS. Patients who received MSCs also reported better quality of life six months later.
“Despite the small number of patients recruited to the trial, we couldn’t have hoped for better results,” said senior author Dr. Stewart, senior scientist at The Ottawa Hospital and professor at the University of Ottawa. “We found MSCs have an important biological effect on these critically ill patients. This shows significant promise and supports further investigation of cell therapy for ARDS.”
Patient grateful to have participated in trial
Kanata resident Sharon Charlebois was recruited to the Phase 1 trial in January 2021 after being admitted to the ICU with COVID-19-associated ARDS.

“I had no problem going into that trial. I didn’t want anyone else to go through what I went through," says Sharon Charlebois.
With dangerously low blood oxygen levels, Sharon was on 100 percent oxygen.
“I remember being asked if I wanted to be resuscitated,” she says. “I must have been quite out of it because I remember thinking ‘Why are you asking me this?’ Dying isn’t something you usually consider.”
She remembers ICU research coordinators Rebecca Porteous and Irene Watpool explaining the cell therapy trial to her. Sharon and her husband agreed it would be a good idea to participate.
“I had no problem going into that trial,” she says. “I didn’t want anyone else to go through what I went through.”
After nine days in ICU and another 13 in hospital, Sharon was very happy to continue her recovery at home. Five years later, she is completely recovered from ARDS.
Local biomanufacturing made trial possible
This therapy couldn’t have been offered to patients like Sharon without The Ottawa Hospital’s Biotherapeutics Manufacturing Centre (BMC).
“In another health emergency, we could restart the trial very quickly because we were able to make the cell product onsite,” said Dr. Stewart. “There’s undeniable power in having this biomanufacturing resource available to ensure that patients benefit from our researchers’ discoveries.”

“We’ve seen that fresh cell therapy is feasible in a pandemic situation, where many patients enroll in a trial relatively quickly, ” says Dr. Dean Fergusson. “We have the expertise and facilities to start this trial again on a dime, if needed.”
As one of the most experienced and successful biomanufacturing facilities in Canada, experts at the BMC worked with the researchers to create a MSC therapy for severe COVID-19-associated ARDS. First, they used cell banks of umbilical cord MSCs from the Center for Regenerative Therapies Dresden in Germany as the starting material. Then they kept fresh cells growing continuously in isolators at oxygen levels similar to the human body. These fresh MSCs were a unique part of the trial.
“The quality and efficacy of cell therapies are highly dependant on how they are processed,” says Eric Lee, General Manager of the BMC. “The cell’s biological activity reflects all the steps it goes through before it’s given to a patient.”
Applications beyond COVID-19
ARDS is responsible for 10 percent of ICU admissions. It has many causes, such as sepsis, influenza and RSV, in addition to COVID-19.

“Despite decades of research, we don’t have great treatments for ARDS,” says Dr. Shane English. “MSCs may be promising if they can regulate the immune system to make the condition less severe.”
“Despite decades of research, we don’t have great treatments for ARDS.” says Dr. Shane English, co-lead author of the study and senior scientist at The Ottawa Hospital and assistant professor at the University of Ottawa. “MSCs may be promising if they can regulate the immune system to make the condition less severe.”
Participants in this trial treated with MSCs showed signs of improvement, but the team doesn’t understand yet why this happened. Their next step is to test patient blood samples to find out how MSCs reversed patients’ dangerously low white blood cell counts. Then they’ll see if tiny particles released by MSCs called exosomes have the same effect. These particles are easier to store and manufacture than living cells.
MSCs may also be a promising tool for future pandemics.
“We’ve seen that fresh cell therapy is feasible in a pandemic situation, where many patients enroll in a trial relatively quickly.” said Dr. Dean Fergusson, co-lead author and Deputy Scientific Director, Clinical Research and senior scientist at The Ottawa Hospital and professor at the University of Ottawa. “We have the expertise and facilities to start this trial again on a dime, if needed.”
Authors:
Shane W. English, Dean A. Fergusson, Manoj Mathew Lalu, David W. Courtman, Saad Khan, Mohamad Sobh, Irene Watpool, Josee Champagne, Samantha Hodgins, Bernard Thébaud, Karim Soliman, Michaël Chassé, Claudia C dos Santos, Marius A. Möbius, Daniel Freund, Mario Rüdiger, Duncan J. Stewart
Funding:
Canadian Institutes of Health Research, the Canadian Stem Cell Network, the Ontario Research Fund, German Federal Ministry for Education and Research.
Core Facilities:
Learn more about:
Media Contact
Amelia Buchanan
Senior Communications Specialist
Ottawa Hospital Research Institute
ambuchanan@ohri.ca
613-297-8315


